
Story
January 13, 2026
People Helping People
Explore how COPO grew out of community need and became a hub for people helping people
Eric Lynch, Chris Lisée

Blog
February 5, 2026
2026 Nonprofit Trends: Challenges, Innovations, and the Capital Needed to Sustain Community Impact
In 2025, I wrote a love letter to nonprofits, thanking them for invaluable contributions to our society during an incredibly difficult time Looking...
Aisha Benson, Annie Chang, David Streim, Dorothy Jones, Jana L Reed, Kristin Giantris, Jennifer Talansky, Jessica LaBarbera, Rakiba Kibria

Blog
January 20, 2026
4 Realistic Actions Funders Can Take Right Now
In a recent blog post, we shared 4 key steps nonprofit leaders can take to manage this moment We now turn to funders – many of whom are asking us a...
Kristine Alvarez

Blog
January 20, 2026
Rooted in Place: What Our Survey Data Found About Nonprofit Real Estate Ownership
By better understanding the factors that influence nonprofit facility ownership, we can make better decisions about how to support nonprofits in...
Elise Miller, Chris Lisée
Filter By:
Story
January 30, 2026
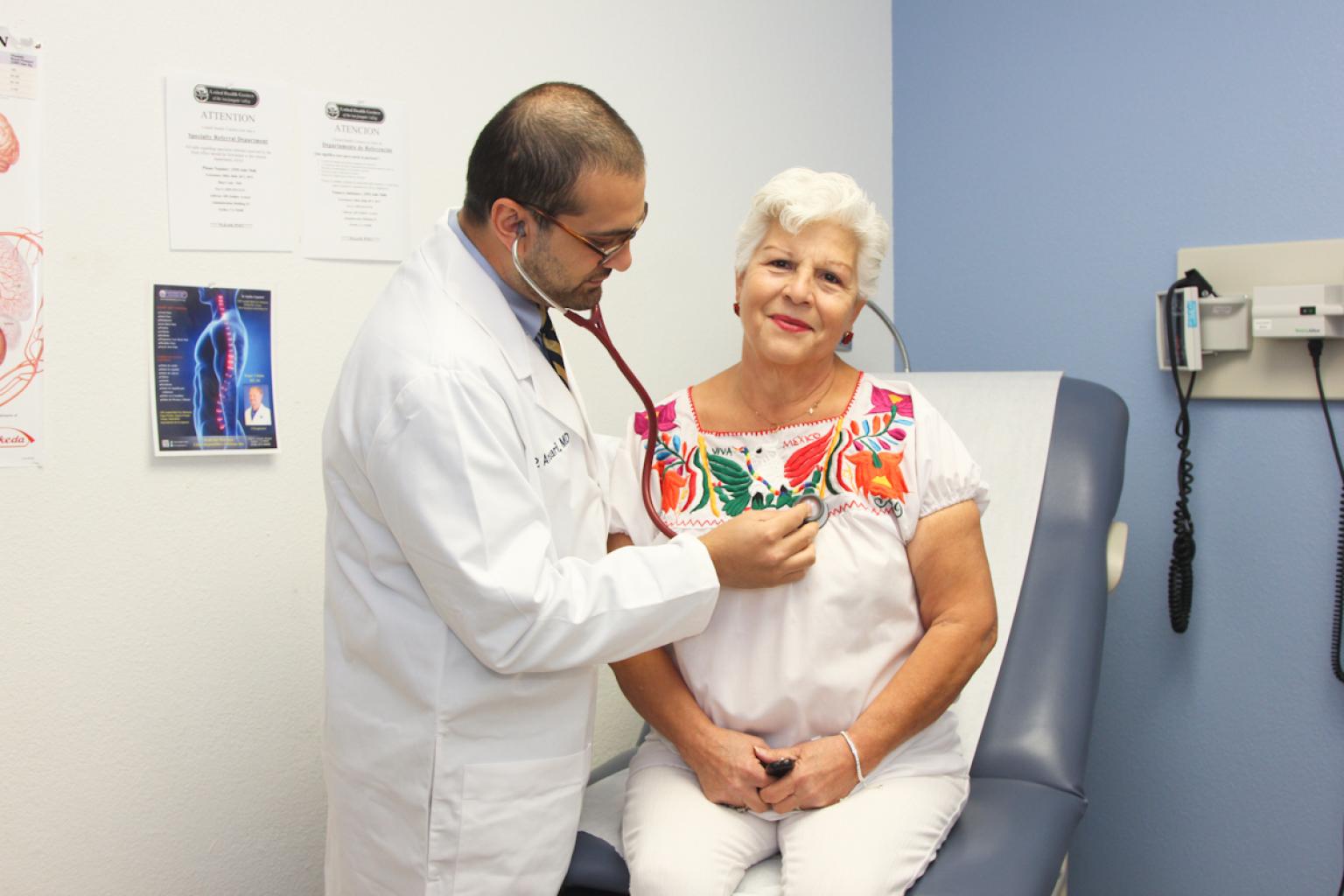
United Health Centers of the San Joaquin Valley: Expanding Healthcare and Opportunity for Older Adults
NFF is proud to finance our first PACE project with United Health Centers of the San Joaquin Valley, deploying $12 million in New Markets Tax Credits...
Janelle Paule

Blog
September 10, 2024
Advancing Team-based Care: A Collaborative Approach
Team-based care (TBC) is an approach to providing holistic healthcare that supports patients by centering them within their care team This...

Projects & Reports
June 10, 2024
The Promise, Pitfalls, and Potential of CalAIM
And what funders can do to ensure the success of this transformational program
Alexandra Chan, Eskedar Getahun
Commentary
April 5, 2024
Connecting with Community-Based Organizations (CBOs): Learning from Failure and Success
Originally published in Medisolv , April 8, 2024 Erin Heilman connected with NFF’s Meadow Didier and Brian Kellaway about the challenges many...
Erin Heilman

Story
June 26, 2023
Columbia River Mental Health Services
“The strength to show up”
Projects & Reports
May 23, 2023
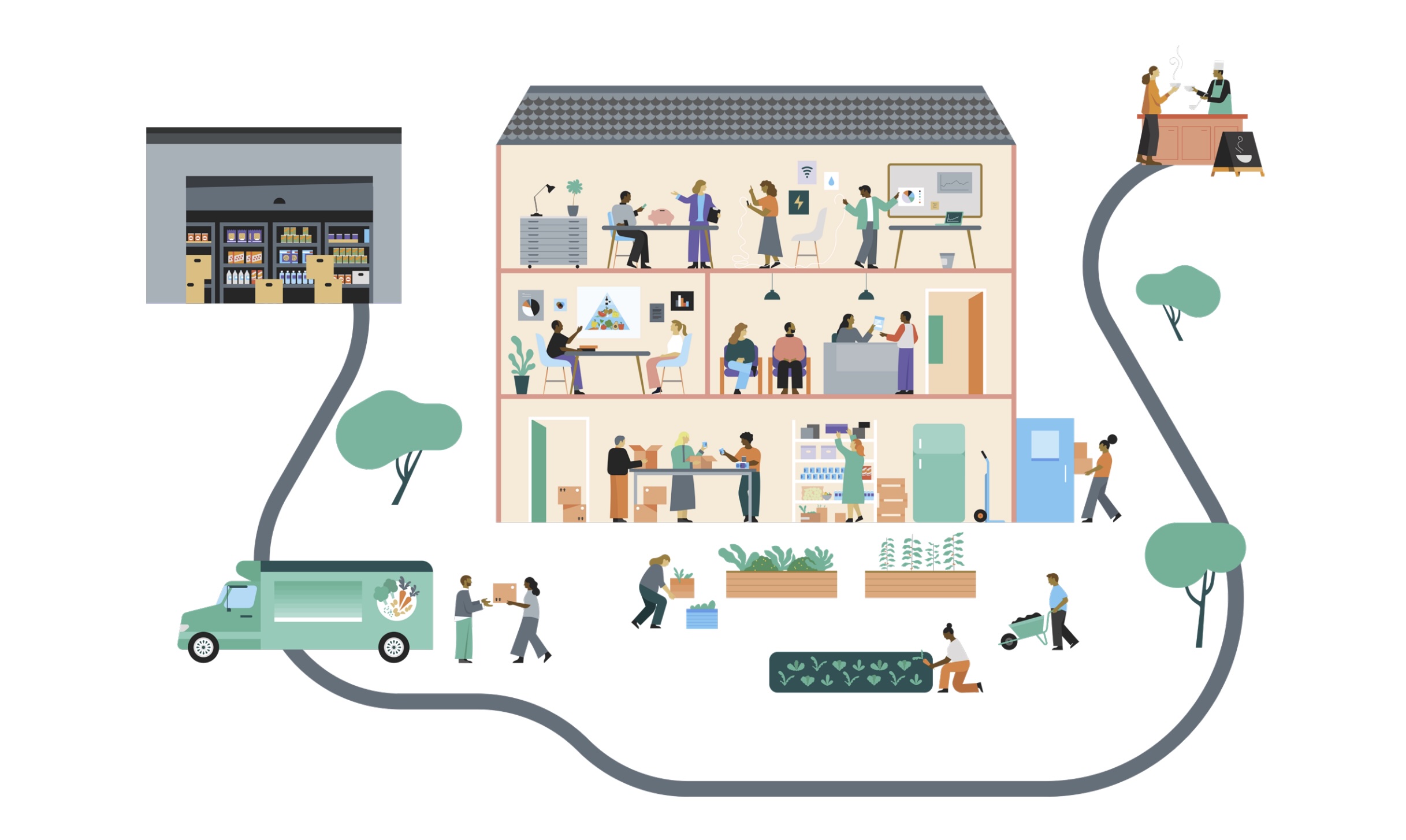
Strengthening the Los Angeles Food Access Ecosystem
Key financial dynamics of and funding opportunities to strengthen the Los Angeles food access ecosystem
Alexandra Chan, Mariesa Kubasek

Story
February 27, 2023
Feed Black Futures
“To feed ourselves, we must free ourselves”
Projects & Reports
June 18, 2021
Advancing Resilience and Community Health
Lessons Learned from Partnerships Between Networks of Community-Based Organizations and Healthcare Organizations The Advancing Resilience and...
NFF Consulting Team

Blog
May 5, 2021
Achieving Health Equity: Community-Led Alternatives to Healthcare-CBO Partnerships
NFF has engaged in numerous efforts across the country focused on facilitating partnerships between community-based organization (CBOs) and health...
Deirdre Flynn
Blog
November 20, 2020
Four Ways to Overcome Partnership Hurdles and Address Social Determinants of Health
Juliette Price is the Chief Solutions Officer for Helgerson Solutions Group, a global consulting firm dedicated to the move to value in health and...
Deirdre Flynn, Juliette Price

Story
October 9, 2020
God’s Love We Deliver
Financial modeling for medically tailored meals
Commentary
April 8, 2020
Who Will Pay for Partnerships that Address Social Determinants of Health?
Originally published in Grantmakers In Health , April 8, 2020 The importance of addressing social determinants of health in driving health outcomes...
Lisa Thirer